Why Point-of-Care Efficiency Affects Your Entire Organization
When you oversee care across dozens of assisted living and memory care communities, small workflow problems rarely stay small. If care teams document late, skip steps, or rely on memory instead of the record, risk builds quietly. Over time, that risk shows up as survey findings, inconsistent care, staff frustration, and difficult conversations after incidents (1, 2).
Point-of-care efficiency is about how easily staff can document care while they are with residents, not after they leave the room. When documentation matches the moment of care, records are clearer, timelines make sense, and expectations are easier to meet. Mobile and tablet-optimized assisted living EHR platforms such as Fynn’s EHR platform are designed around this reality rather than around fixed desks and shared computers.
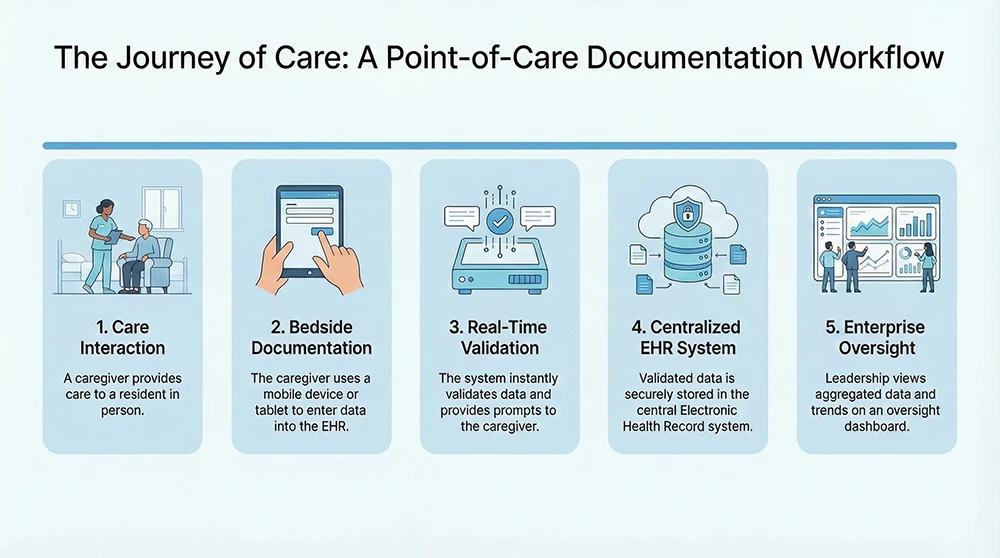
What Point-of-Care Efficiency Looks Like in Senior Living
In assisted living and memory care, efficiency means staff can access resident information, record care, and note changes without leaving the resident environment. You want documentation to happen in resident rooms, dining areas, or common spaces, not hours later at a workstation (3).
Senior living also has unique constraints. Many frontline caregivers are not licensed nurses. Turnover is higher than in other healthcare settings. Regulations differ by state and often change (4). These factors make delayed documentation risky. Mobile EHR tools work within these limits by supporting staff where they are, both physically and skill-wise.
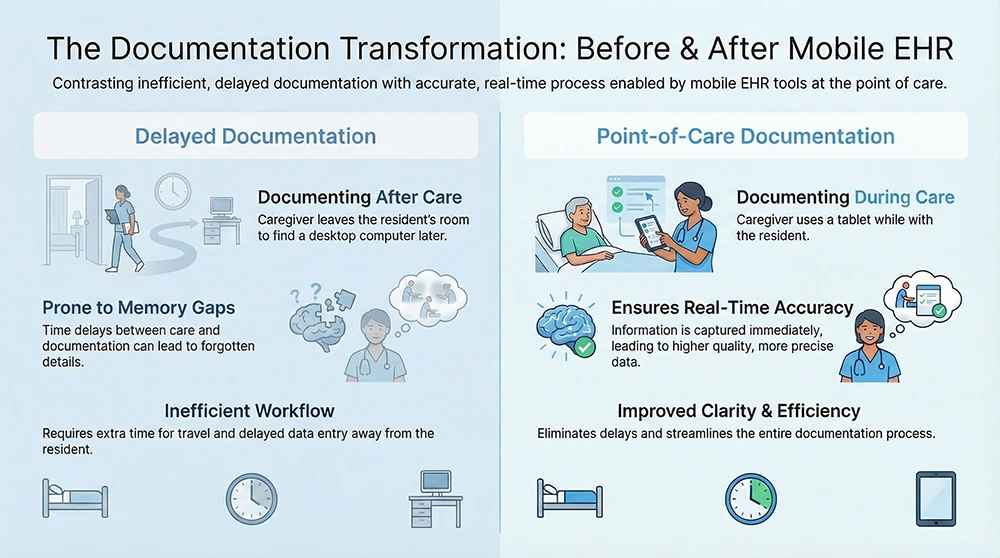
How Mobile EHRs Improve Documentation Accuracy
When staff complete care first and document later, details fade. Time stamps blur. Important observations may never make it into the record (5). Mobile EHR tools reduce this gap by letting staff document in real time or immediately after care.
In memory care, this matters even more. Behaviors, mood shifts, and safety risks can change quickly. When staff document these changes as they happen, the care record reflects reality instead of a summary written from memory (6). Over time, this leads to more reliable care plans and stronger continuity between shifts.
You also reduce reliance on verbal handoffs. When staff can see care plans, diagnoses, and recent notes on a tablet, they do not have to guess or ask around. Communication breakdowns are a known cause of adverse events, and real-time access lowers that risk (7).
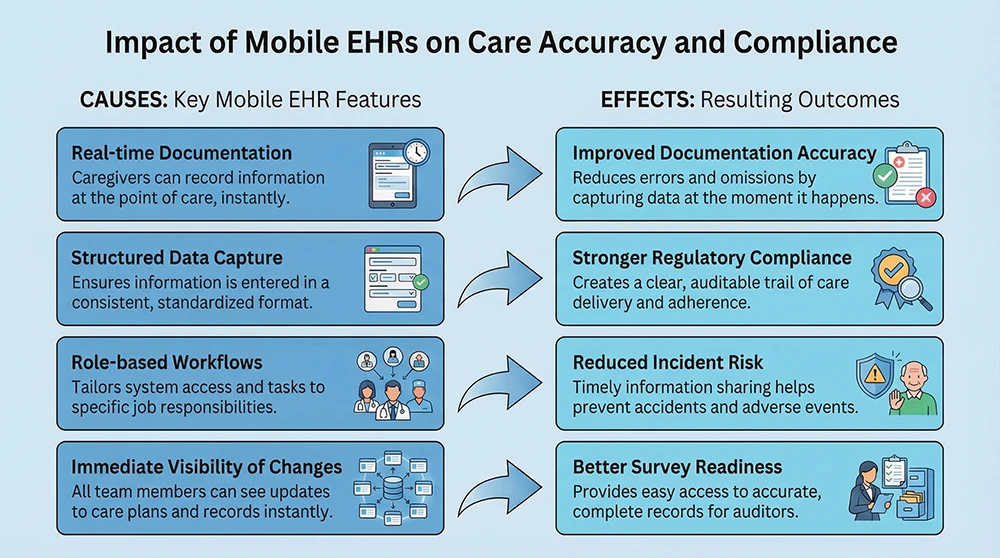
Making Compliance Easier at the Point of Care
Mobile-optimized assisted living EHR platforms often use role-based workflows. Caregivers see caregiver tasks. Nurses see nursing tasks. Each role is guided through the documentation required for that moment of care (8).
This approach matters because assisted living regulations require specific documentation, but frontline staff are not expected to know regulatory language by heart (9). Mobile EHRs act as built-in reminders. Required fields, prompts, and task lists help ensure nothing important is missed.
Structured documentation also supports consistency across communities. While narrative notes still matter, structured fields make audits, surveys, and internal reviews easier to manage (10). For you, this means fewer surprises when regulators arrive and clearer insight into where support is needed.
Giving Staff More Time for Residents
Point-of-care documentation reduces the total time staff spend charting compared to delayed documentation models (11). When staff document as they go, they spend less time retracing steps or trying to remember details at the end of a shift.
That time savings often shows up as better resident supervision and engagement. Families notice when staff are present instead of focused on paperwork. Regulators notice, too, because quality of life is part of the compliance picture (12).
Mobile EHR tools also help with onboarding. Assisted living and memory care experience high turnover (13). When workflows are clear and easy to follow, new hires reach competency faster and make fewer documentation errors.
Improving Communication Across the Care Team
When documentation happens at the point of care, changes in condition become visible to the rest of the team quickly. Nurses, supervisors, and leaders can see what happened and when it happened without waiting for end-of-shift notes (14).
In memory care, early visibility can prevent hospital transfers. Small changes often signal bigger problems. When those changes are documented promptly, the care team can respond sooner (15).
For you as a Corporate Wellness Director, mobile documentation feeds enterprise reports and dashboards. This allows you to spot patterns, compare communities, and intervene before problems grow (16). Point-of-care efficiency supports proactive oversight instead of reactive management.
Supporting Multi-State Compliance
Assisted living regulations vary widely by state, especially around assessments, service plans, medication documentation, and incident reporting (17). Mobile EHR platforms configured for senior living can enforce state-specific requirements during daily care activities.
This approach improves survey readiness. Documentation shows clear timelines and consistent follow-through. When complaints or incidents occur, records are easier to review and defend (18, 19). For organizations operating across several states, this consistency reduces risk at scale.
Reducing Risk Through Timely Incident Documentation
Falls, elopements, and behavioral incidents remain among the highest-risk events in assisted living and memory care (20). Mobile EHR tools allow staff to document incidents immediately, while details are still clear.
Early documentation also triggers follow-up steps such as assessments, notifications, and care plan updates. Over time, this creates better data for quality improvement efforts. When documentation is timely and consistent, trend analysis becomes more reliable (21).
Practical Considerations for Adoption
Mobile EHR adoption requires planning. Devices must be secured, access must be role-based, and data must be protected under HIPAA requirements (22). Training also matters. Staff adoption improves when tools fit real workflows and expectations are reinforced by leadership (23).
Your role is central. When you set documentation standards and use data to guide decisions, mobile tools become part of daily practice rather than another system staff try to work around.
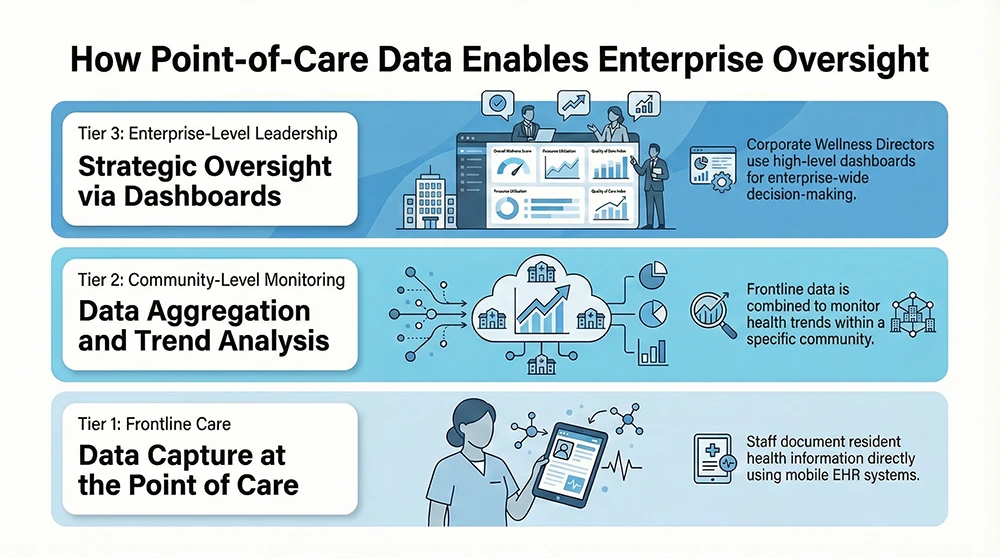
What This Means for You as a Corporate Wellness Director
Mobile and tablet-optimized EHR platforms support standardized care, compliance, and oversight across large portfolios. They help you see what is happening at the point of care without being physically present in every community.
By improving point-of-care efficiency, you strengthen documentation, reduce risk, and give care teams tools that match how they work. That alignment supports better outcomes for residents, staff, and the organization as a whole.
Conclusion
Mobile and tablet-optimized EHR tools improve point-of-care efficiency by allowing documentation to happen where care happens. For assisted living and memory care leaders, this leads to clearer records, stronger compliance, reduced risk, and better visibility across communities. As care complexity grows, point-of-care technology becomes a practical requirement, not a nice-to-have.
References
- Centers for Medicare and Medicaid Services, State Operations Manual
- Office of Inspector General, Adverse Events in Assisted Living
- Agency for Healthcare Research and Quality, Health IT and Patient Safety
- National Center for Assisted Living, Assisted Living Facts and Figures
- AHRQ, Improving Documentation Accuracy
- Alzheimer’s Association, Dementia Care Practice Recommendations
- Joint Commission, Sentinel Event Data Root Causes
- HIMSS, Usability in Health IT
- National Association of State Regulatory Agencies, Assisted Living Regulation Overview
- CMS, Surveyor Guidance for Assisted Living Providers
- Journal of Nursing Administration, Point-of-Care Documentation and Efficiency
- CMS, Quality of Life in Long-Term Care
- Bureau of Labor Statistics, Healthcare Turnover Data
- AHRQ, Care Coordination Measurement Framework
- Journal of the American Geriatrics Society, Early Detection of Change in Condition
- HIMSS, Data Analytics in Senior Care
- National Conference of State Legislatures, Assisted Living Policy Trends
- CMS, Enforcement Actions in Assisted Living
- State Survey Agency Training Materials
- Centers for Disease Control and Prevention, Falls in Older Adults
- Institute for Healthcare Improvement, Quality Improvement in Long-Term Care
- HHS Office for Civil Rights, HIPAA Security Rule Guidance
- AHRQ, Health IT Implementation Best Practices
Disclaimer:
This article provides general information for educational purposes and does not constitute legal, regulatory, financial, or compliance advice. Assisted living and memory care regulations vary widely by state and may change without notice. Requirements related to HIPAA, cybersecurity, documentation, and electronic health records depend on your organization’s structure, payer relationships, billing methods, and operational practices.
You should consult qualified legal counsel, regulatory specialists, or state licensing authorities to determine the specific obligations that apply to your communities and to verify how the guidance in this article relates to your organization’s compliance responsibilities.








%2520(1).jpeg)